Beyond Mechanical Maladaptation: The Neurochemical Framework of MdDS
Mal de Debarquement Syndrome (MdDS) represents one of the most persistent diagnostic and therapeutic challenges in vestibular medicine. While the field has historically approached this condition as a primary mechanical maladaptation of the “vestibular ocular reflex” (VOR) and velocity storage, recent theoretical models suggest that we must expand our scope to include the underlying neurochemical environment of the brainstem.
The Neurochemical Instability of the Brainstem
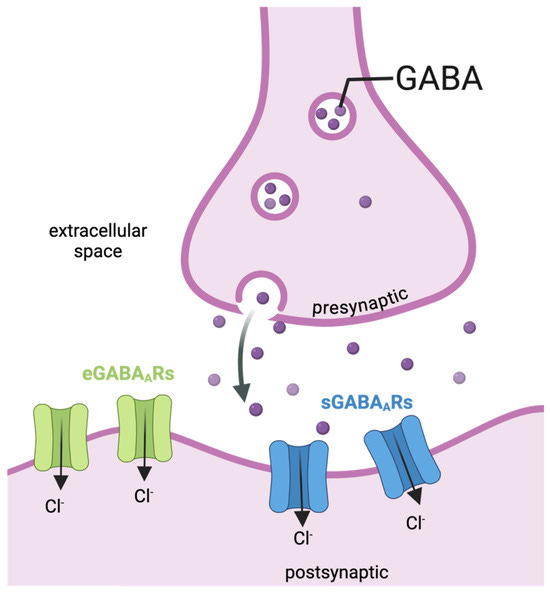
The brainstem nuclei responsible for integrating velocity storage signals rely on a high density of “GABAb-sensitive neurons”. These neurons function as the critical “stop” signal, dampening vestibular activity once a stimulus ceases. In MdDS patients, this inhibitory control appears to fail, locking the velocity storage system into a perpetual state of signal integration.
This is where the role of “Calcitonin Gene-Related Peptide” (CGRP) becomes essential to our clinical understanding. CGRP, an inflammatory neuropeptide well-documented in the pathophysiology of migraine and depression, acts as a modulator of these “GABAb-sensitive neurons”. When CGRP levels become aberrant—often triggered by gonadal hormonal fluctuations—the resulting neurochemical environment may override the inhibitory dampening required to cease signaling. Consequently, the patient remains trapped in a feedback loop of phantom motion (Mucci et al., 2018).
Clinical Relevance: Why This Matters for Your Patients
For the vestibular professional, this framework shifts the patient management strategy from mere compensation to optimizing the central vestibular microenvironment.
Validation of Symptom Persistence: Many patients report that their sensations do not match their physical exam findings. This neurochemical model provides a physiological basis for their symptoms, explaining that the issue lies not in the peripheral sensory organs but in the brainstem's failure to “reset” due to an unstable inhibitory environment.
Identifying High-Risk Profiles: Patients with comorbid migraine or depression are not just experiencing unrelated issues; they are likely manifesting a baseline instability in their “serotonergic” and “GABAergic” systems. These patients should be viewed as higher risk for developing chronic MdDS following motion exposure.
Optimizing Multidisciplinary Care: Recognizing this framework empowers you to move beyond exercise-based protocols. If the primary driver is a CGRP-mediated signaling failure, vestibular exercises alone may be insufficient. Collaboration with neurologists to explore the use of “CGRP antagonist” drugs may provide the necessary medical support to “optimize” the environment, thereby enabling your rehabilitation strategies to be effective (Mucci et al., 2018; Zhang et al., 2023).
The Path Forward
As we refine our clinical approach, we must treat MdDS as a condition of systemic neurochemical integrity. Our goal is to “coordinate” rehabilitation with medical strategies to address the brainstem's metabolic landscape. By recognizing the interplay between “GABA” and “CGRP”, you can provide your patients with a clearer explanation of their condition and a more targeted, multidisciplinary path toward recovery.
References
Mucci, V., Jacquemyn, Y., Van Ombergen, A., Van de Heyning, P. H., & Browne, C. J. (2018). A new theory on the involvement of GABA and Calcitonin Gene-Related Peptide in Mal de Debarquement Syndrome: predisposition factors and pathophysiology. Medical Hypotheses, 120, 128–134. https://doi.org/10.1016/j.mehy.2018.08.024
Zhang, Y., Zhang, Y., Wang, Y., Zhang, X., Qin, G., Zhang, D., Chen, L., & Zhou, J. (2023). Inhibition of glutamatergic trigeminal nucleus caudalis-vestibular nucleus projection neurons attenuates vestibular dysfunction in the chronic-NTG model of migraine. The Journal of Headache and Pain, 24(1). https://doi.org/10.1186/s10194-023-01607-z