Beyond the Straight Line: Unleashing Global Torque with Circular Dot Optokinetic Flow in Mal de Debarquement Syndrome (MdDS)

Before you read this article, please, take a deep breath. It is a bit complex but crucial in understanding the use of external optokinetics to induce movement in your patient. If you do not understand this, please reread it. If it remains challenging, feel free to email me to discuss further. (bwerner27811@gmail.com)
Navigating Complex Maladaptations with Advanced Visual Strategies
As vestibular therapists, we routinely encounter the profound disorientation of Mal de Debarquement Syndrome (MdDS). It's a condition that leaves patients and, frankly, many clinicians feeling adrift in a world that refuses to stop rocking. While Dr. Mingjia Dai and his team at Mount Sinai pioneered the groundbreaking optokinetic stimulation (OKS) protocol, offering a beacon of hope, its precise application for complex cases demands a deeper, more nuanced understanding.
The initial success of the Dai protocol primarily utilized linear optokinetic stripes, moving horizontally or vertically, to induce a targeted vection.
This was revolutionary. However, some MdDS patients defy such precise, uni-directional categorization. Their sensations of motion feel chaotic, encompassing forward-backward bobbing, side-to-side swaying, and even turning—an authentic 'moving all over' experience. For these individuals, relying solely on a single-axis linear OKS might prove insufficient to compel a global recalibration.
This necessitates a deep dive into the profound potential of circular dot optokinetic flow—a method that is not just a continuation of the Dai protocol, but a significant leap forward. It is capable of inducing a more comprehensive sensory challenge and leveraging both active and passive torque to compel central nervous system reintegration. This advanced approach aligns with the continuous evolution of vestibular science, including ongoing research at leading centers such as Mount Sinai.
The Deep Dive: Circular Dot Optokinetic Flow for a Global Challenge
When we encounter a patient with MdDS symptoms that manifest as a truly 'moving all over,' spiraling, or ambiguous sway, the shortcomings of relying solely on linear OKS become evident. While linear stripes offer targeted correction for distinct directional biases, they may not provide the robust or comprehensive input needed for these diffuse, multi-planar maladaptations. This underscores the need for a more comprehensive approach, such as circular dot OKS.
This is precisely where circular dot optokinetic flow becomes essential.
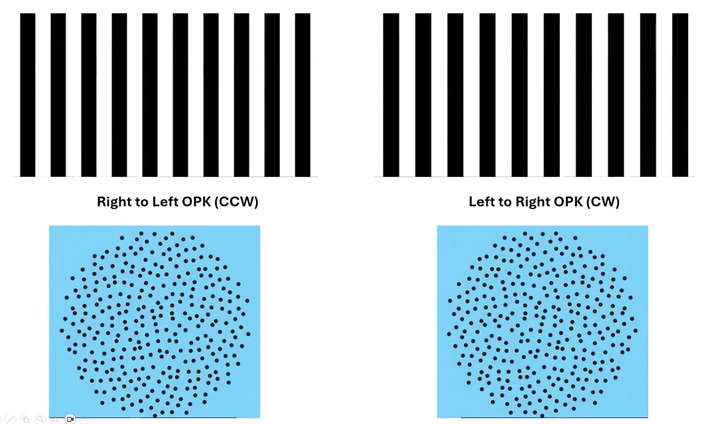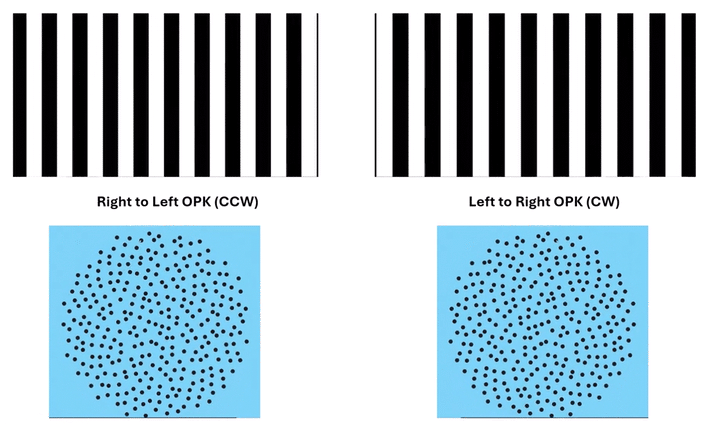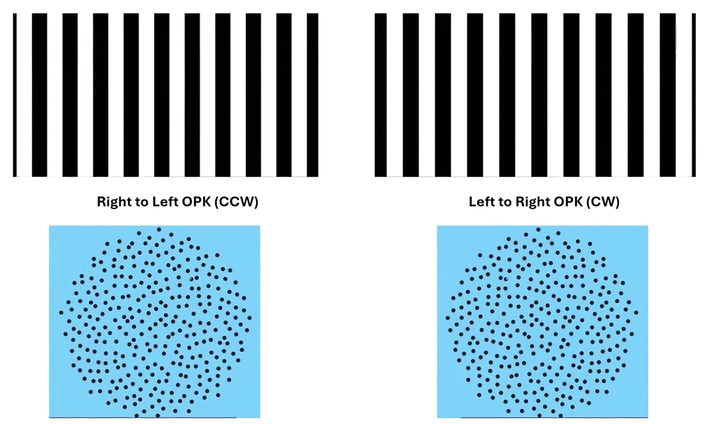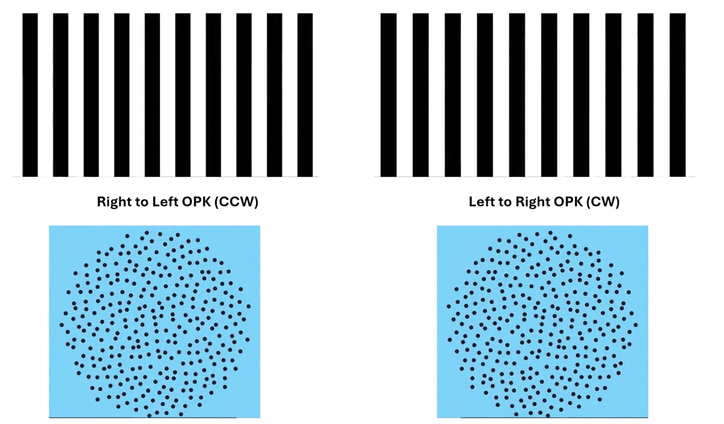
These dynamic visual stimuli—whether rotating clockwise or counterclockwise, or contracting—offer a fundamentally different approach. They simultaneously present visual motion cues across all planes: horizontal, vertical, and oblique. This comprehensive approach reassures us that we are addressing a complex, pervasive central maladaptation. The presence of circular OPK dots on the Mount Sinai MdDS site strongly suggests their use in this evolving clinical landscape, signifying a recognition of their unique advantages.
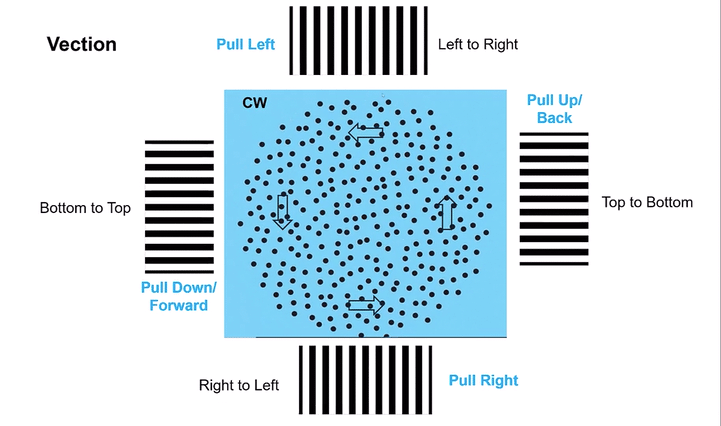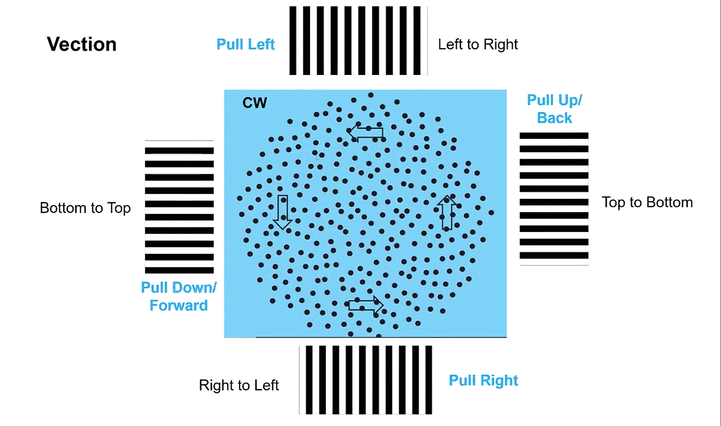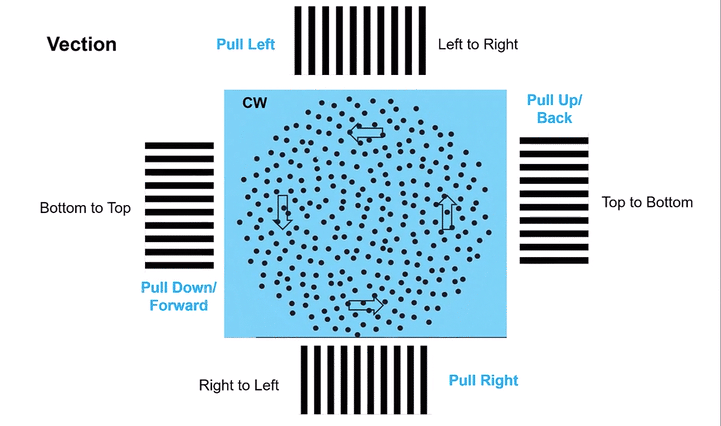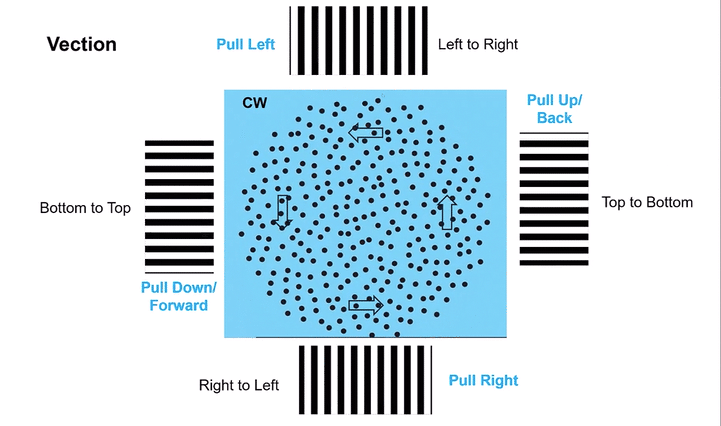
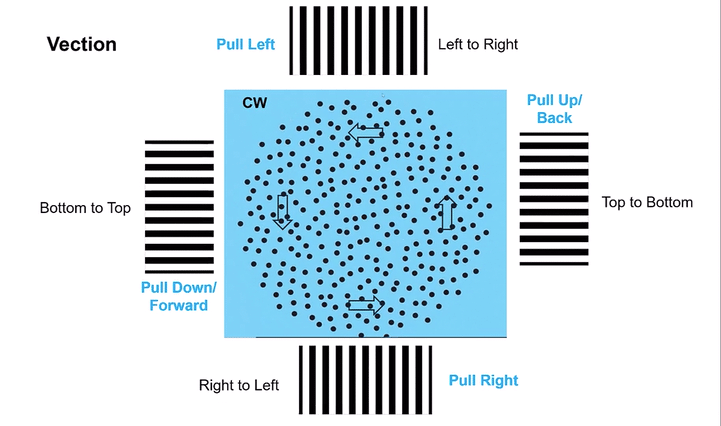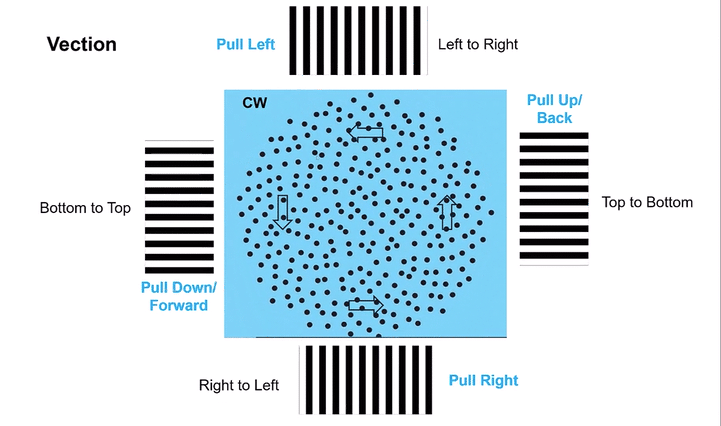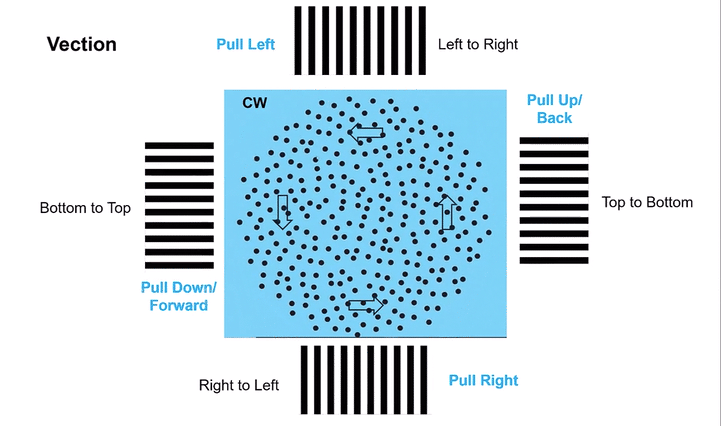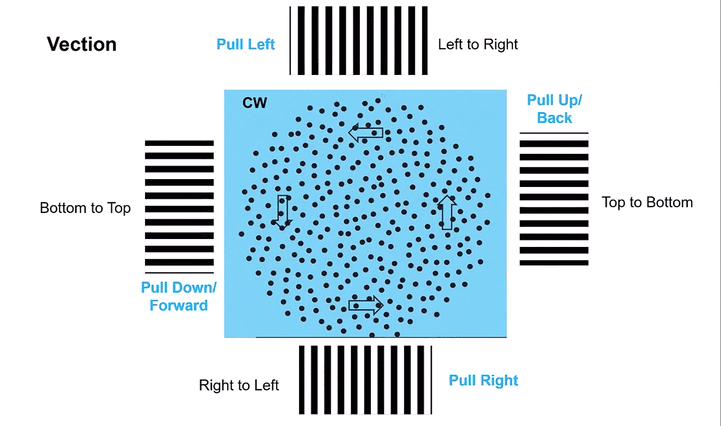
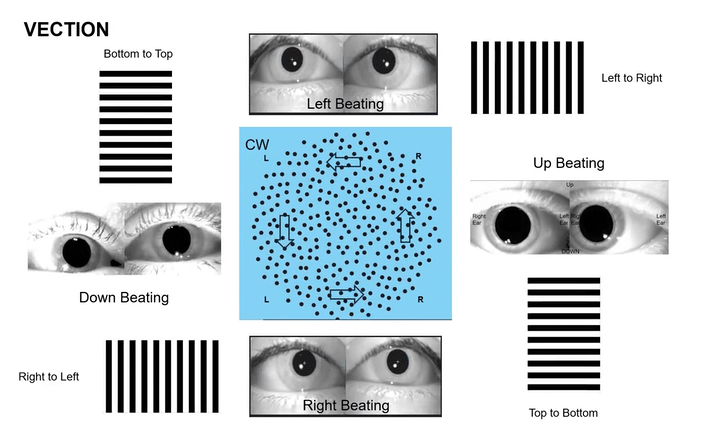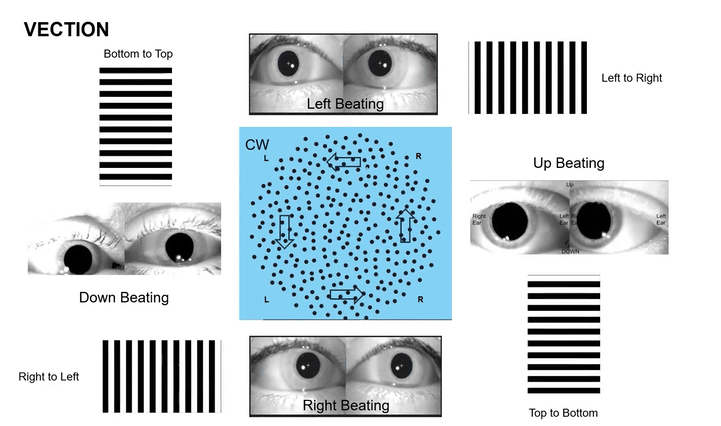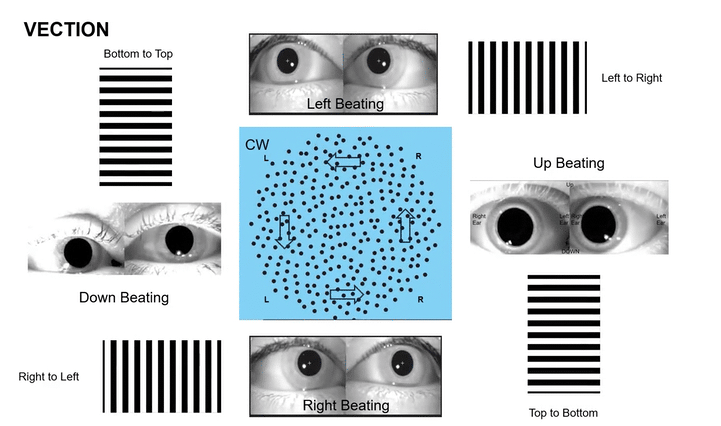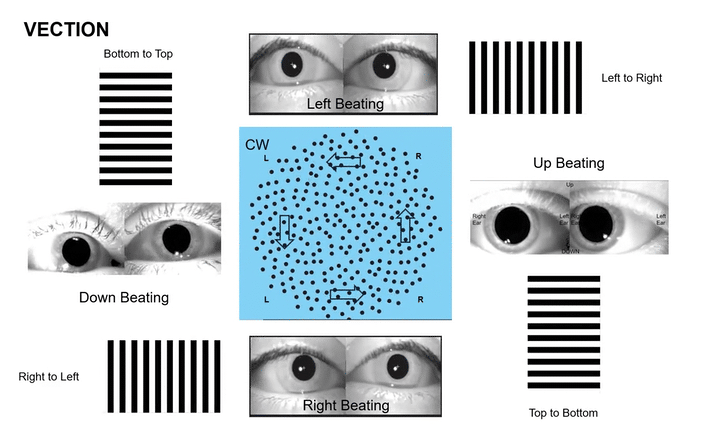
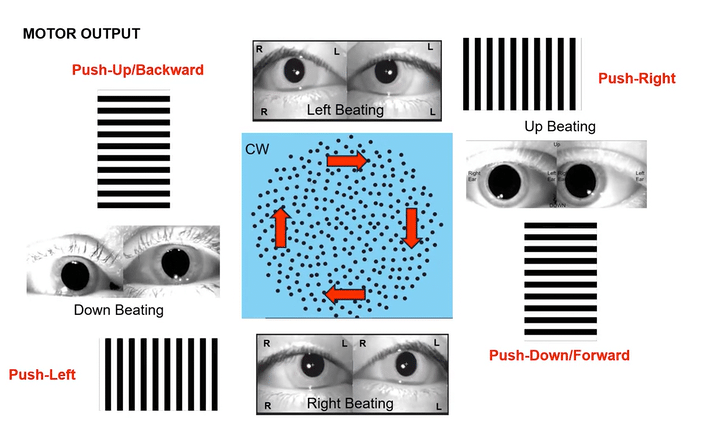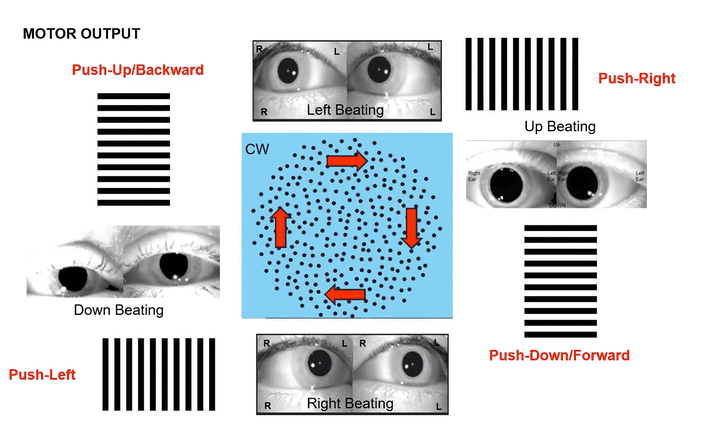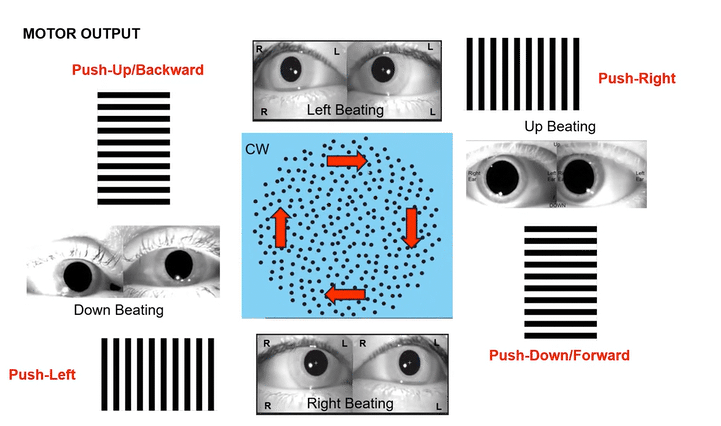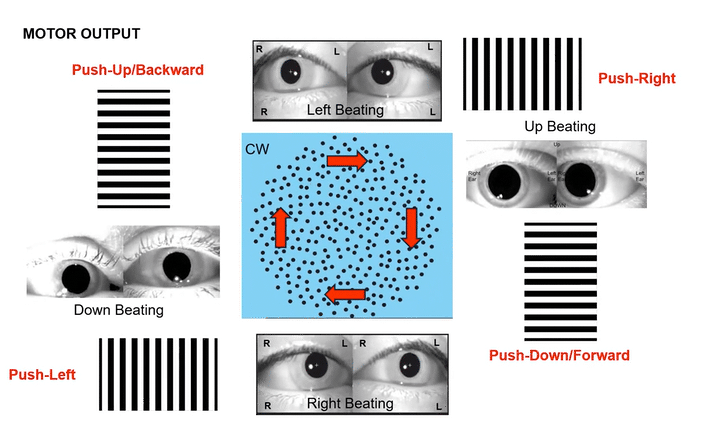
Omni-Directional Vection & Motor Output: Circular dots inherently induce a sensation of self-motion (passive torque) that has both rotational and often translational components in multiple directions simultaneously. This creates a pervasive illusion of motion. For instance, looking at a clockwise circular dot pattern:
The top section (dots moving left to Right) induces a Left-Beating Nystagmus and a perceived leftward vection.
The right side (dots moving Top to Bottom) induces an Upbeat Nystagmus and a perceived backward vection.
The bottom section (dots moving Right to Left) induces a Right-Beating Nystagmus and a perceived rightward vection.
The left side (dots moving Bottom to Top) induces a Downbeat Nystagmus and a perceived forward vection.
This nuanced, multi-directional vection then elicits complex, global active postural responses, as the body naturally tries to stabilize itself against this comprehensive visual challenge.
Addressing the 'All Over' Problem: When a patient feels they are 'moving all over,' it logically follows that we provide the central nervous system a stimulus that is also 'all over,' but in a controlled, therapeutic manner. We consciously choose to induce a stimulus that mirrors the complexity of their maladaptation, driving a more comprehensive reset.
Leveraging Both Passive and Active Torque: A Controlled Overwhelm
The actual therapeutic potential of circular dot OKS, especially for patients with a diffuse sensation of motion, lies in its capacity to harness both passive and active components of torque, creating a controlled overwhelm. This ‘controlled overwhelm’ is designed to force reintegration, and it's this control that should give us confidence in the therapeutic potential of this technique.
Passive Torque (Vection) Remains Primary: The patient must primarily observe the whole field of dots passively. This is the core of the MdDS 're-trick, as it creates the direct conflict between perceived motion and actual stillness. It keeps the body still, theoretically, while the brain processes the illusion, thereby supporting the critical re-adaptation process without confounding inputs from active bodily movement. This commitment to 'super simple', targeted input ensures the clearest message to the brain.
How to Instruct for Passive Vection: You would guide the patient in a step-by-step manner:
'I need you to look at the screen, but don't try to focus on any single dot. Think of it like looking out a car window, but not trying to read the signs as they go by. I want your eyes to be soft, almost as if you're looking through the dots, letting the whole field of movement just wash over you.'
You might add: 'Let your eyes go with the flow of the dots, but don't actively try to chase them. Just allow them to move your eyes naturally.'
Always couple this with: 'Remember, your job is to keep your body as still as possible. You might feel like you're moving, but you know you're not. Let your body remain calm and still, while your eyes take in this movement.'
Directions for Passive Vection:
If a predominant rotational sway exists (e.g., they feel continuously turning left/right), you would typically start with the circular rotation (CW or CCW) that induces a vection opposite to their perceived rotational sway.
For genuinely 'all over' or ambiguous sway, alternating between clockwise and counterclockwise rotation across trials or sessions becomes essential. This provides comprehensive, multi-planar stimulation.
Dot Parameters (Density & Speed): These are titrated based on patient tolerance and therapeutic response. Your system's ability to offer different vections—Clockwise, Counterclockwise, Up, Down, Right, Left, Forward—provides unparalleled control. Begin with moderate density and tolerable speed, gradually increasing to maximize the therapeutic challenge while avoiding excessive distress. The presence of these circular OPK dots at centers like Mount Sinai underscores this evolving approach.
Active Torque (Motor Output/Pursuit) as a Complementary Layer: While less central to the initial velocity storage reset, consciously engaging in active pursuit of elements within the circular dot pattern can offer an additional, powerful therapeutic layer. Suppose the observer actively follows the dots in a clockwise circular optokinetic flow, consciously tracking elements as they move. In that case, everything is indeed in reverse compared to the direction induced by passive vection. Active pursuit directs the perceived and attempted motion in response to the stimulus.
How: Instruct the patient to 'actively pick a single dot or section and follow it' as it moves around the circle, or to 'actively track the flow of dots' in a specific direction. This engages higher cortical centers and creates a direct, volitional motor output.
Rationale: This contributes to 'controlled overwhelm,' which forces deeper neural computation for reintegration. It pushes the brain harder, especially for complex or later-stage cases, or if passive vection alone proves insufficient.
By combining these elements—a pervasive passive vection (illusory motion in all four directions, including complex rotational/translational components) with the potential for active visual pursuit (deliberately engaging in tracking within that multi-directional field)—we barrage the central nervous system with a rich, complex, and intensely compelling amount of sensory input. This isn't about simply making the patient sicker than a dog; it's about providing a therapeutic intensity that demands recalibration.
The Comorbidity Factor: Not a Vacuum
It's crucial to remember that patients do not exist in a vacuum. While MdDS is a distinct entity, many patients present with co-occurring vestibular disorders, whether peripheral or central. I have found a significant number of MdDS patients also have vestibular migraines (which can affect both central and peripheral systems), underlying central sensitivities, or even unique neural systems and personality types—like the brilliant, motivated, and highly engaged Type A individuals I commonly see (doctors, executives, and other high-achievers are frequent presentations)—that might predispose them to developing such complex neural conditions. These comorbidities add layers, but the core principle of recalibrating the velocity storage through targeted passive vection often remains the primary therapeutic aim for the MdDS symptoms.
Conclusion
Mastering optokinetic torque for MdDS means embracing the power of the 'Keep It Super Simple' approach. We leverage passive visual input to induce compelling illusions of motion, forcing the brain's maladapted velocity storage to confront and resolve a critical sensory conflict. By understanding this precise mechanism and trusting keen clinical observation over rigid adherence to potentially misleading tests, we can genuinely help our MdDS patients escape the torment of constant motion and find their stable ground again.
About the Author: Brian K. Werner, PT, MPT
Brian K. Werner, PT, MPT, Cert. L3-MBR is the National Director of Vestibular Education & Training at FYZICAL, and a highly accomplished physical therapist widely recognized for his expertise in balance and vestibular disorders. With over a quarter of a century of experience, Brian has dedicated his career to revolutionizing balance rehabilitation. His passion for helping patients with dizziness and balance challenges stems from his background as a gymnast and a traditional rock climber. These experiences instilled in him a deep understanding of balance, coordination, and movement. Brian's innovative contributions to the field include the development of the Safety Overhead Support System (SOS). This pioneering solution allows patients to challenge their balance systems at the highest functional levels safely. He has treated tens of thousands of patients with balance and vestibular disorders, and his insights continue to shape advanced treatment paradigms across the country and across the world.



Wow! A deep breath indeed. That was a lot to take in, but thanks for putting it out there.