Optimizing Postural Stability: The Role of Adaptive Surface Cueing in Vestibular Rehabilitation
In the clinical management of complex vestibular disorders, we often encounter a common physiological hurdle: the sensory mismatch. Whether treating patients with Persistent Postural-Perceptual Dizziness (PPPD), Mal de Debarquement Syndrome (MdDS), or Bilateral Vestibular Hypofunction (BVH), the core challenge remains the same—the central nervous system cannot resolve conflicting orientation cues. This leads to the characteristic maladaptive sensory strategies we see daily: high visual dependence, trunk stiffening, and a profound loss of the vestibulospinal reflex.
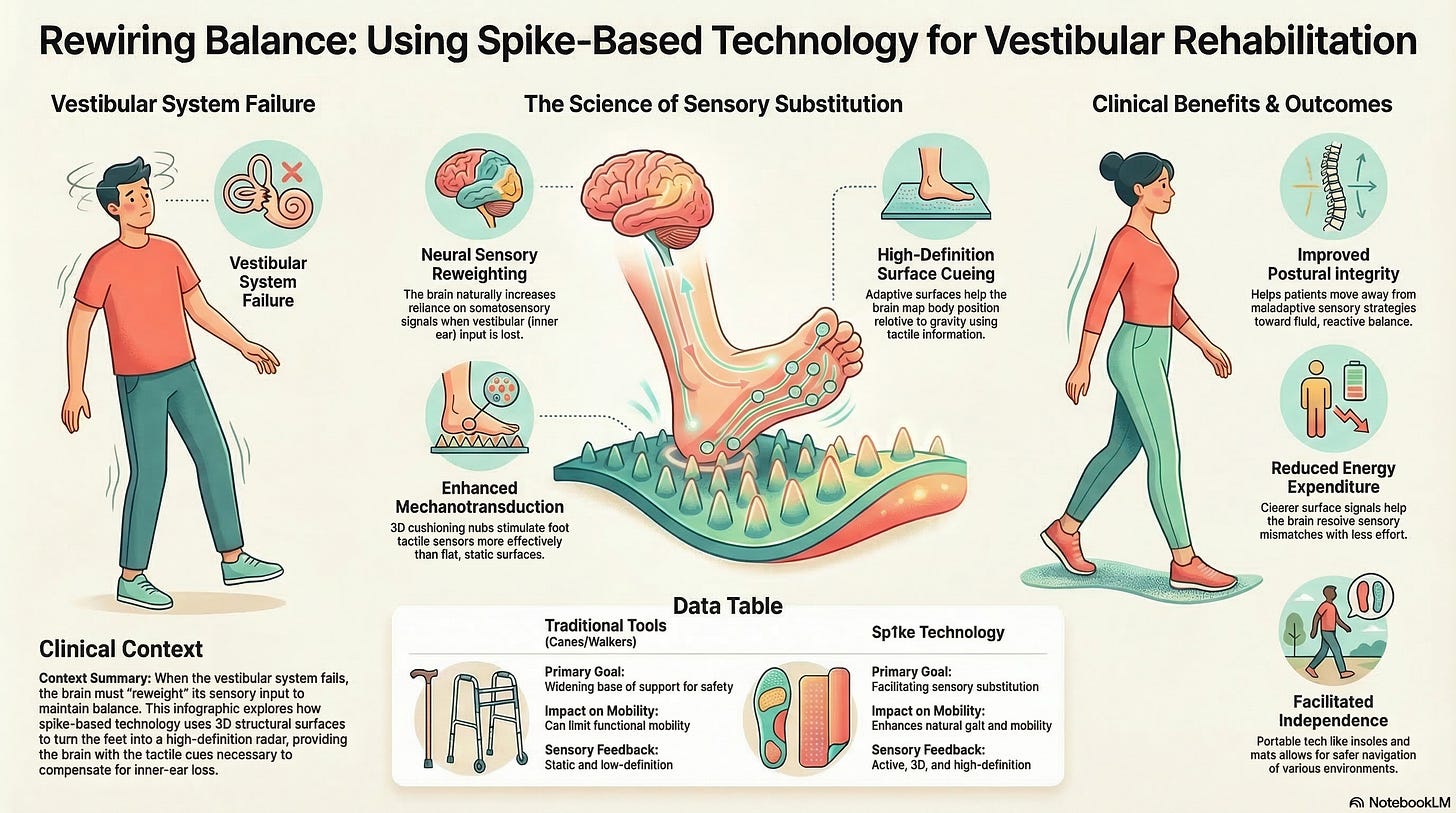
The emerging science of ergomorphology and spike-based technology, specifically through Vigurus Technologies and its Sp1ke products, offers a sophisticated means of facilitating sensory substitution. Rather than relying on static surfaces or assistive devices that can limit mobility, this technology improves the interface between the body and the environment, turning every point of contact into a high-definition radar system for the brain.
The Mechanism of High-Fidelity Surface Input
For patients with bilateral loss or senior citizens at high risk for falls, the brain must “up-weight” somatosensory signals to compensate for compromised vestibular data. Traditional foam or rubberized materials are often too static; they provide comfort but do not actively communicate spatial changes. Sp1ke technology employs a globally patented structural surface composed of hundreds of mini cushioning nubs and connected bendable rods that move in 3D space.
This design facilitates rehabilitation through several key mechanisms:
Enhanced Mechanotransduction: The flexible nubs stimulate mechanoreceptors and tactile sensors more effectively than flat surfaces. This helps the brain map the body’s position relative to gravity-related tactile information.
Cortical Facilitation: Research confirms that when vestibular input is compromised, the brain naturally increases its reliance on online steering and orientation cues from other systems (Clemens et al., 2011).
Proprioceptive Salience: Textured surfaces improve postural stability by increasing sensory feedback from the skin (Nabavi et al., 2023). This is crucial for seniors and patients with unilateral deficits who need to “re-anchor” their center of gravity.
Clinical Application Across the Vestibular Spectrum
This technology is not limited to foot orthotics. It serves as a global postural tool that can be integrated into every phase of the rehabilitation process:
PPPD and MdDS: These patients often suffer from a “sensory mismatch.” The Sp1ke surface provides thousands of independent touchpoints that give the brain a clear, undeniable “ground truth.” This helps the patient down-weight visual triggers and reduce the “walking on marshmallows” sensation.
Bilateral Loss and Senior Fall Prevention: For those with a complete loss of vestibular-spinal function, the mats and insoles provide the constant, adaptive queuing necessary to maintain independence without the drag of traditional mobility aids.
Supine and Floor-Based Integration: Using these mats during early-phase exercises helps patients engage sensory integration through their remaining vestibular function and vision. The dense data set provided to the spinal and trunk muscles helps coordinate vestibulospinal pathways before the patient even stands.
Facilitating Independence and Mobility
For the vestibular professional, the goal is always to provide sufficient input to ensure safety without sacrificing the patient's remaining mobility. Sp1ke products are composed of a closed-cell EVA foam that returns energy rather than trapping the patient, supporting a more natural movement pattern.
By transitioning from static stability to an active, adaptive surface, we can:
Coordinate Better Postural Integrity: Helping patients move away from rigid, guarded movements and toward fluid, reactive balance.
Reduce Cognitive Load: When the brain receives clear, reliable surface cueing, it spends less energy resolving sensory mismatch, reducing the systemic exhaustion common in chronic dizziness.
Facilitate Full-Body Integration: Whether using a mat in the shower, a pad on a treatment table, or insoles in walking shoes, this technology provides a portable, therapeutic aid for any environment.
Clinical Conclusion
The potential for spike-based technology to facilitate sensory substitution is a significant development in our field. By improving the signaling environment, we can provide our patients with the tools they need to stay active and grounded.
If you are interested in exploring how to integrate this into your clinical practice, you can find more information on Vigurus Technologies' website. Please feel free to mention that Brian Werner referred you. I am eager to hear from other professionals regarding their clinical observations with this technology across various patient populations.
References
Clemens, I. A., De Vrijer, M., Selen, L. P., Van Beuzekom, A. D., & Medendorp, W. P. (2011). Multisensory integration in online steering. Journal of Neurophysiology, 105(4), 1533–1548. https://doi.org/10.1152/jn.00760.2010
Hirase, T., Inokuchi, S., Matsusaka, N., & Okita, M. (2015). Effects of a balance training program using a foam rubber pad in community-based older adults: a randomized controlled trial. Journal of Geriatric Physical Therapy, 38(2), 62–70. https://doi.org/10.1519/JPT.0000000000000021
Nabavi, S., Hadian, M. R., Olyaei, G., Talebian, S., & Shabanloei, R. (2023). Immediate effect of textured insoles on the balance in patients with diabetic neuropathy. Journal of Diabetes Investigation, 14(3), 456–463. https://doi.org/10.1111/jdi.13965



I have used the Sp1ke mats in our vestibular clinic for 3 or more years as well as the Sp1ke insoles. I do find them appropriate with some of our patients and greatly enjoy working with the Sp1ke family. Brian Jamieson is incredibly brilliant and kind!