The Unexpected Vertigo: When Routine Ear Cleaning Shakes More Than Just Wax

As a physical therapist specializing in vestibular disorders, I frequently encounter presentations that highlight the intricate sensitivity of our balance system. One intriguing phenomenon involves vestibular disruption following routine ear cleaning, a scenario worth exploring for its diagnostic and therapeutic implications.
Consider a clinical example: a patient presents with sudden, profound vertigo immediately following an ear irrigation procedure performed to clear wax. Often, this involves warm water lavage, sometimes preceded by a wax-softening agent like Debrox. This acute onset of dizziness, persisting beyond the immediate procedure, offers a compelling case for investigation.
The Pseudo-Caloric Phenomenon
This immediate, intense dizziness points directly to a caloric response.
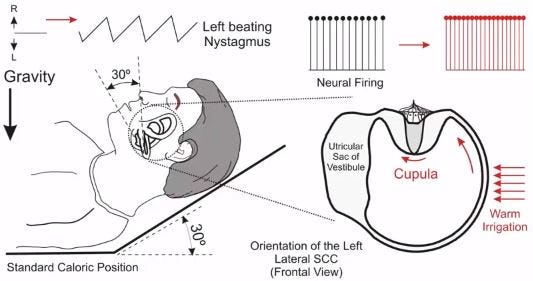
What Does Caloric Mean in This Context? When we discuss a caloric response in the ear, we refer to a test or phenomenon that uses temperature changes to stimulate the inner ear's balance organ. The inner ear, specifically the semicircular canals, contains fluid (endolymph). When warm or cold water (or air) enters the ear canal, it creates a temperature gradient that causes this fluid to move. This fluid movement then stimulates the nerve endings in the canal, which sends a signal to the brain indicating head movement, even if the head is perfectly still. ENT doctors intentionally perform caloric tests to assess inner ear function, but an accidental temperature change from a procedure like a warm water ear lavage can also induce this intense sensation of vertigo and dizziness. It powerfully demonstrates how sensitive our balance system is to even slight changes in its environment.
In cases involving ear irrigation, the warm water inadvertently triggers this robust response. It acts as a pseudo-irritation of the vestibular system, mimicking the effects of a diagnostic caloric test. Clinicians may observe prolonged dizziness in patients after formal caloric tests, where the ear's delicate balance mechanism temporarily becomes hypersensitive or partially impaired.
For more information on how ear irrigation can sometimes lead to dizziness, clinicians can review resources like this one: Ear Irrigation (Ear Lavage) - Healthgrades. This phenomenon, where the temperature of the water can influence the inner ear, is well-documented in medical literature.
The Age Factor and Compensatory Challenges
An important aspect influencing the severity and persistence of symptoms in such cases often relates to patient age. For instance, in an individual in their early nineties, the central nervous system's capacity for rapid vestibular compensation frequently diminishes. Younger, healthier systems more readily adapt to acute vestibular insults. However, for an older adult, this sudden, unexpected caloric stimulus from an ear irrigation can lead to prolonged disequilibrium, severe imbalance, and functional decline because their brain struggles to compensate for the sudden, false signal effectively. This impaired compensation contributes significantly to persistent symptoms like unsteadiness and increased fall risk.
Differentiating Persistent Imbalance: Beyond BPPV
Crucially, this type of calorically induced imbalance may persist beyond the immediate procedure, significantly impacting mobility and functional independence. While Benign Paroxysmal Positional Vertigo (BPPV) often enters the differential diagnosis given a history of positional dizziness, a thorough objective assessment is essential. Employing tests such as the Dix-Hallpike Test and Supine Head Roll Test with infrared video oculography (IVOG) allows for a definitive ruling out of BPPV. Observation of mild nystagmus may occur, but without the specific characteristics or symptom provocation associated with BPPV. This confirms that ongoing symptoms stem from a more generalized irritation or temporary dysfunction of the inner ear, rather than otoconia displacement.
Further objective insights often come from Instrumented CTSIB (FYZICAL-CTSIB) testing. Results frequently reveal patterns such as a Somatosensory>Visual-Vestibular Mismatch (SVVM). This indicates an over-reliance on input from somatosensory cues (feet, ground), with compromised integration of visual and vestibular information. This explains profound instability and persistent instability.
Navigating the Modern Medical Landscape
This clinical scenario highlights a challenging aspect of our current medical model. Routine procedures, sometimes performed in primary care settings by ancillary staff, may inadvertently impact nuanced and delicate systems like the inner ear. While ear wax removal is standard, the potential for an adverse vestibular reaction, particularly in older adults with diminished compensatory capacity, emphasizes the interconnectedness and fragility of our sensory systems.
The Path to Recovery: Skilled Vestibular Rehabilitation
Despite the challenging onset, this condition responds well to skilled physical therapy intervention. A focused course of vestibular rehabilitation targets the specific sensory mismatch identified during assessment. Treatment plans aim to:
Re-calibrate the patient's balance system.
Reduce reliance on assistive devices.
Significantly lowers the risk of falls.
Improve overall functional independence and quality of life.
Therapists systematically challenge balance through customized home exercise programs, progressively re-exposing the system to movements that facilitate neural adaptation and compensation. While recovery requires dedication, significant gains in stability and confidence are achievable. Recognizing and properly diagnosing this pseudo-caloric phenomenon allows us to provide targeted and effective care for improved patient outcomes.
Brian K. Werner, PT, MPT, has been a physical therapist specializing in vestibular issues for over a quarter of a century and is the National Director of Vestibular Education & Training at FYZICAL.